The skin is the largest organ in the body and serves a number of important functions that keep you alive and healthy. It is also deceptively complex and, like every other organ in your body, it requires care and maintenance to ensure it is kept in top condition.
The main function of skin is to form a protective barrier around the body which shields you from the elements like intense sunlight or rain. Without it, bacteria and other germs would be able to enter your body and cause infections. It also helps to hold in body fluids to make sure you do not get dehydrated.
The skin also plays an important role in temperature regulation in the body. It keeps in body heat when you are cold, and glands in the dermis layer of your skin release sweat to stop you from overheating when the ambient temperature gets too high.
Skin Diseases
As the body’s first line of defence against the external environment, our skin is constantly exposed to changing conditions. This can result in a number of skin disorders which present as rashes, dry skin, acne, inflammation, itchiness, abnormal pigmentation, and scaly skin. These disorders can range from mild to severe and may have varied causes that may require a consultation with a dermatologist to confirm.
Your skin is also impacted by what happens inside your body. Hormonal changes can affect the quality of skin and lead to conditions like acne. Autoimmune diseases can also cause your immune system to attack healthy skin tissue to cause psoriasis, scleroderma, and a number of other conditions.
Bacterial buildup on your skin, fungus, and parasites can all cause health issues. Certain people with pre-existing conditions are at higher risk of such skin infestations. This group includes diabetics, the elderly, patients with HIV, hepatitis, or other immune disorders.
Skin that is inflamed due to disease or damaged by trauma is more prone to get infected. Any break in the skin can expose a person to infection that can progress to cellulitis and sepsis, which is potentially life-threatening.
An In-depth Look Into Common Skin Diseases

Acne: Symptoms & Causes
Acne is a skin disorder which most would have experienced at least once. It occurs more frequently during puberty and during periods of hormonal changes. Some patients may struggle with chronic acne for decades and might require frequent visits to dermatologists.
Acne happens when hair follicles become clogged with oil or dead skin cells. For those who have acne, their body produces too much of an oily substance known as sebum. Ordinarily, sebum locks moisture in your skin, protects your skin from UV radiation, and repels bacteria. However when too much sebum is produced, the excess mixes with dead skin cells to plug up hair follicles.
This plugged follicle then ends up bulging outwards to form either whiteheads or blackheads. An open pore leads to blackheads as it has been exposed to air and become oxidised, turning it dark coloured. A closed pore becomes a whitehead as the sebum and dead skin cells retain their natural colour.
Bacteria that live on the skin can then contaminate and infect the plugged follicles, causing papules, pustules, nodules or cysts which can be very noticeable during an acne flare up.
Acne symptoms are fairly obvious and can be diagnosed via a visual examination. Acne can occur in any place on the body but it is usually seen on the face, shoulders, upper back, and chest.

Crusting, cysts, papules, pustules, scarring, whiteheads, and blackheads are usually the visual indicators that skin specialists and dermatologists look out for when diagnosing acne. The severity of acne can be classified as mild, moderate, or severe, depending on the number and type of acne spots present.
Overproduction of sebum that leads to acne is linked to a number of causal factors. At the top of the list is hormonal changes like increased amounts of androgens, which are a group of sex hormones. Androgens include hormones like testosterone and they help start puberty. This is the reason why teenagers undergoing sexual maturity are the group most strongly associated with acne.
However, hormonal changes do not only happen during puberty. Menstrual cycles, pregnancies, menopause, and even stress can all cause hormonal spikes that can cause or worsen existing acne symptoms.
Steroid medication, lithium, and certain epilepsy drugs can also cause acne as a side effect. In many cases it may not be desirable to stop the medication, and as a result patients might have to turn to standard acne treatments in Singapore to manage the side effects. Talk to your healthcare provider first before starting any acne medication.
Acne also has a genetic component. While there is no specific acne gene, if one or both your parents had acne then there is a higher chance that you might develop acne too. Keep in mind that other factors such as diet and environment also affect the quality of your skin and may play a role in how prone you are to acne breakouts.
Learn More: Understanding Adult Acne: Common Causes & Treatments Available
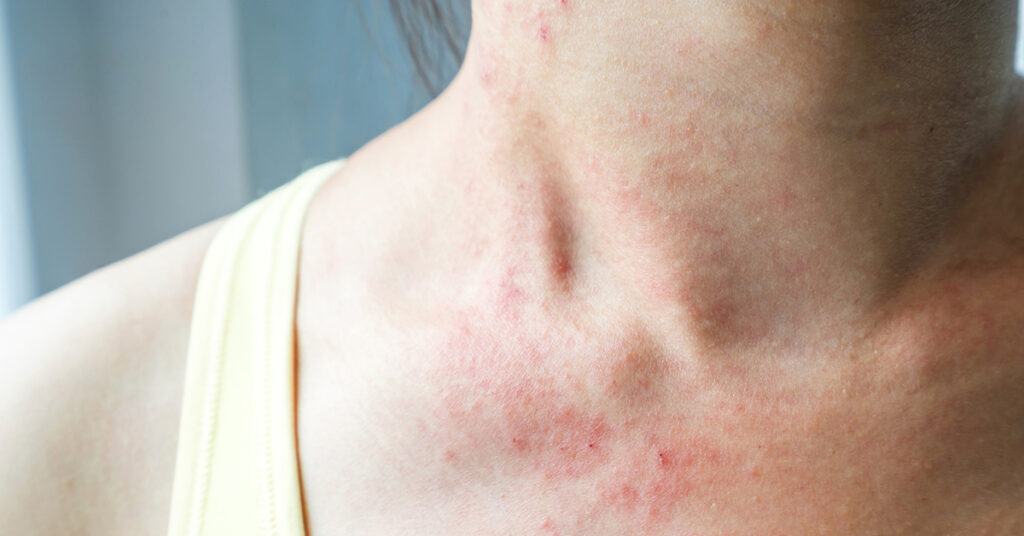
Atopic Dermatitis: Symptoms & Causes
Atopic dermatitis, commonly referred to as eczema, is a condition that causes dry, itchy, and inflamed skin. Symptoms can appear anywhere on the body and present as cracked skin, rashes, raised bumps, oozing, thickened skin, sensitive skin, and general skin itchiness.
Diagnosis of atopic dermatitis is done through an examination of the affected areas, and talking to the patient about their family medical history. Often other causes of symptoms such as allergies and other skin diseases will have to be ruled out before eczema treatment is prescribed.
Atopic dermatitis is widespread among the population with an estimated 20% of children and 11% of adults affected by this condition. It is not contagious and cannot spread to others. It can however weaken your skin barrier and make you more susceptible to skin infections, something that eczema sufferers have to be careful about. Especially when scratching the affected areas as this can cause the skin layers to break.
There are many different causes and triggers for atopic dermatitis. External factors include the surrounding environment, allergens, certain fabrics, dry air, sweat, and temperature. These can all cause skin irritation and dry out the top layer of skin which can worsen eczema symptoms.
Other contributing factors for atopic dermatitis include genetics, immune responses, stress, anxiety, and depression. If you inherit certain genes from your parents, you are more likely to develop eczema later in life.
People might find that their eczema flares up more often when they are stressed or anxious. This is due to certain hormones like cortisol and adrenaline. These hormones can suppress the immune system and increase inflammation throughout the body and in the skin.
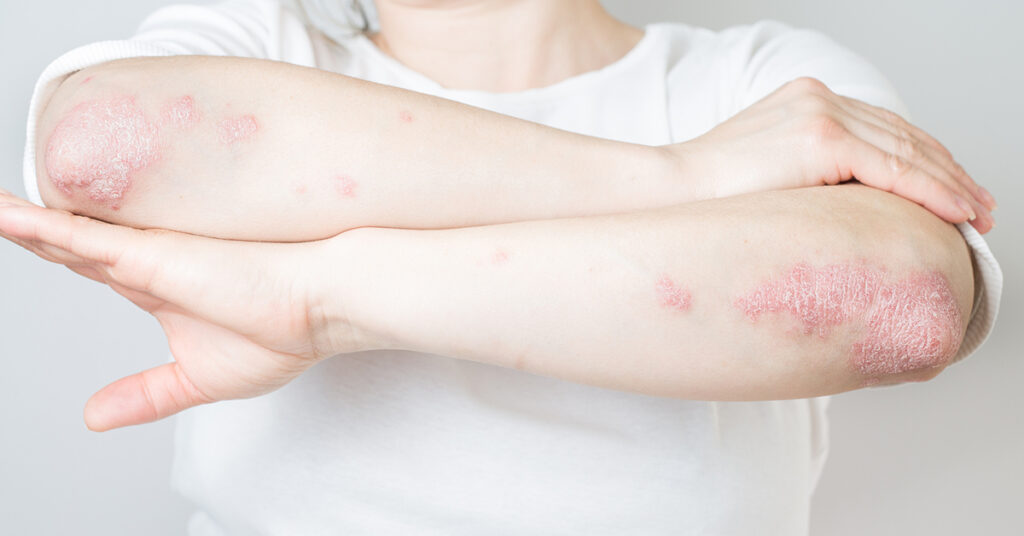
Psoriasis: Symptoms & Causes
Psoriasis is a skin disorder that causes flaky, itchy patches of skin which can form scales. These patches can appear anywhere on the body but are most often found on the elbows, knees, scalp, and lower back. They can also vary widely in appearance from individual to individual.
There are several different types of psoriasis which are diagnosed by signs and symptoms. The most common type is known as plaque psoriasis which is identified by scaly, raised patches of skin.
Another form of psoriasis is known as nail psoriasis and it primarily affects fingernails and toenails. It causes pitting, abnormal nail growth, and discoloration. Severe nail psoriasis may even cause the nail to crumble.
A psoriasis diagnosis can be confirmed by your dermatologist clinically. Occasionally, a skin biopsy is performed if the features are not classical, in order to exclude other conditions that may mimic psoriasis. Some of the differences between psoriasis and eczema are the areas each disorder is usually found at, intensity of itchiness, and appearance of symptoms. Psoriasis appears in different areas and tends to be less itchy than eczema.
The causes of psoriasis are not fully understood. The condition is not contagious but can be triggered by environmental factors like infections, weather, injury, alcohol consumption, medications, and withdrawal from corticosteroids. Psoriasis is a chronic condition like atopic dermatitis and people may be symptom-free for years before encountering a trigger that sets off the disease.

Hyperpigmentation: Symptoms & Causes
Hyperpigmentation is a term that refers to patches of skin that are darker than the surrounding skin. It can happen on any part of the body and is usually due to an increase in melanin production in a specific area. It can occur in small areas, cover large patches of skin, or even affect the entire body.
The three main types of hyperpigmentation are sunspots, melasma, and post-inflammatory hyperpigmentation. The most common form of hyperpigmentation are sunspots.
Sunspots are also known as liver spots or solar lentigines. As the name implies, it is triggered by exposure to the sun. Sunlight stimulates production of melanin as the role of melanin is to protect your body from the sun’s harmful UV rays. However overexposure to sunlight may lead to uneven melanin creation which results in hyperpigmentation.
Learn More: How To Prevent Sun Spots?
Sun exposure can also exacerbate hyperpigmentation from other causes. Sunspots are generally harmless but what you assume to be a sunspot might turn out to be a cancerous mole. It is always advisable to get any new and sudden development of hyperpigmentation checked out by a dermatologist.
Melasma is a hyperpigmentation skin condition that is often found among pregnant women and is more likely to be found in females than males. It usually presents as freckles and blotchy spots on the face and may be symmetrical.
The root cause of melasma is suspected to be hormonal. Darker skinned individuals or people who have a tendency to tan are more susceptible to melasma and hyperpigmentation in general. Oestrogen and progesterone sensitivity is associated with the condition and it has been linked with birth control pills, hormone therapy, stress, and thyroid disease.
Learn More: Skin And Hair Changes During Pregnancy
Post-inflammatory hyperpigmentation happens when there is injury to skin or trauma. After the skin has healed, it may leave behind a flat area of discoloured or hyperpigmented skin. It can be found anywhere on the body where skin healing has occurred. Skin conditions like acne and eczema can often leave behind post-inflammatory hyperpigmentation patches.
The reason behind post-inflammatory hyperpigmentation is thought to be due to skin cells increasing melanin production as a response to damage or irritation. If however a pigment spot is changing colour, size, shape, or is itching or bleeding, then a dermatologist should be visited to rule out other skin disorders.
Treatment Options For Common Skin Diseases

Oral Medications
Medications that can be taken orally have been shown to have good efficacy against a number of different skin disorders. Antibiotics can be used for moderate to severe cases of acne as a measure to reduce bacteria on your skin causing the acne. These have to be prescribed by a trained dermatologist and might be combined with other medications to prevent antibiotic resistance. They can also cause side effects like increased sun sensitivity. Pregnant women and young children are often recommended not to take oral antibiotics.
Oral contraceptives are another option for acne treatments. They work by regulating androgen levels to lower the stimulation of sebum production. Females with acne along their jaw and the lower half of their face often see good results with this treatment. There are however side effects like weight gain, breast tenderness, and nausea.
For eczema sufferers, the range of oral medications include short courses of systemic steroids (frequent or long-term use should be avoided), and other oral immunosuppressive therapy if the condition is severe.
Oral immunosuppressives can be prescribed for psoriasis sufferers who have not responded to other forms of treatment or have more severe cases of psoriasis. One example are retinoids which are pills used to reduce the production of skin cells, the major issue implicated in psoriasis. These drugs should not be taken by pregnant or breastfeeding women.
Biologics
These are a group of medications that target certain proteins and molecules and are effective in treating eczema and psoriasis. Dupilumab is a monoclonal antibody that targets interleukins 4 and 13 and has been shown to be very effective for moderate to severe cases of atopic dermatitis. The range of biologics for psoriasis is even wider, and your dermatologist will discuss the various options with you. These biologics have shown high efficacy in clearing skin lesions and treating arthropathy associated with psoriasis.

Topicals
Topicals like creams, gels, and lotions are often the first line of treatment for patients with skin issues like acne and eczema. Applied directly to the affected area, they can be highly effective in solving a number of skin issues.
Vitamin A derived retinoids help to unclog pores and hair follicles, reduce inflammation, slow down skin cell growth, and are often used for patients with moderate acne and plaque psoriasis. They also have other skin health benefits but can cause side effects like dryness, redness, and sun sensitivity.
Antibiotics and salicylic acid kill excess skin bacteria and reduce redness and inflammation. They can be combined with retinoids for greater effect, although a dermatologist should always be consulted beforehand. Just like oral antibiotics, topical antibiotics are often paired with benzoyl peroxide to reduce antibiotic resistance.
Corticosteroid creams can be used to combat the itching symptoms that come from eczema and help to repair your skin. They reduce inflammation, suppress overactivity of the immune system, and constrict blood vessels. Other conditions which can be treated by steroid creams are psoriasis and contact dermatitis, which causes dandruff and scaly patches on skin. Patients need to be careful with steroid creams for eczema treatment and not overuse the medication.
If you have milder forms of eczema, you can opt for non-steroidal anti-inflammatory topicals. These work by blocking specific enzymes and regulate inflammation in your skin. The advantage with such topicals is that they do not have the more severe side effects associated with steroid creams.
Laser Treatment for Hyperpigmentation
Lasers can be an effective form of treatment for most forms of hyperpigmentation. The lasers work by shattering the melanin pigments into smaller pieces which are then removed by your skin’s natural process of renewal. In addition to reducing hyperpigmentation, laser treatments for your face can also leave your skin brighter and smoothen out uneven tones.
There are many different lasers and each one can also be precisely calibrated depending on the patient’s condition and extent of hyperpigmentation. Your dermatologist will be able to determine if your skin requires deeper or shallower penetration for optimal results. You will also likely need multiple treatments over several weeks.
The two main types of laser treatments for pigmentation involve non-ablative and ablative lasers. Non-ablative lasers can destroy melanin producing cells without damaging the skin surface. Ablative lasers remove the top layer of skin and can also help with acne scars.
While there are pros and cons to both types of lasers, for laser treatments to be truly effective, the patient has to ensure that they care for their skin after the procedure. Simple tips like staying out of the sun, keeping the skin clean and moisturised, and staying away from cosmetic products can make all the difference.
Learn more: Caring For Your Skin After A Laser Treatment For Pigmentation
Common Questions You May Have
1) Can picking at acne scars make the problem worse?
Yes, picking at acne scars can worsen your acne. It can make the skin around your acne red and inflamed, the pimple may bleed or develop into a scab, and can lead to an infection due to the bacteria on your hands and surrounding skin. It can also result in acne scars which stay on your face permanently unless you opt for laser treatments for your face or other dermatological procedures.
2) When should I see a doctor about my skin condition?
For simple skin problems, you can visit your primary care doctor for over-the-counter prescriptions. However, if your skin condition covers a large part of your body, does not respond to other treatments, or it presents with other symptoms like fever, joint aches or muscle pain, then it is definitely time to make an appointment with a skincare specialist.
You should also visit a dermatologist if you have chronic skin conditions like atopic dermatitis, psoriasis, or moderate to severe recurrent acne.
3) How are skin diseases diagnosed?
Many skin diseases can be diagnosed visually by a trained eye. For those that cannot be diagnosed in this way, your dermatologist might perform a skin biopsy by removing a small patch of affected skin to study under a microscope.
Other diagnostic methods include diascopy, which involves pressing a microscope slide against the skin and applying pressure to see if it changes colour, and using a device called a dermatoscope to diagnose skin lesions.
4) Are there health conditions that put me at higher risk of developing skin issues?
If you have other pre-existing medical conditions like diabetes, inflammatory bowel disease (IBD), or lupus, you may be at higher risk of developing skin issues. For diabetes, this is linked to higher sugar levels in your blood. IBD and lupus are multisystemic autoimmune diseases that can affect the skin.
5) What lifestyle tips can I adopt to prevent skin issues?
Just like any other organ, good lifestyle habits can do wonders for skin health. Getting good quality sleep, reducing stress, and eating a healthy diet are all ways to improve your skin and overall physical health.
Using appropriate sunscreen and staying away from harsh cosmetics are two specific lifestyle tips you can adopt to prevent skin issues from flaring up.
Learn More: 4 Good Habits For Healthy Skin
6) Do skin conditions return after treatment?
Many skin conditions are chronic and have no cure. Psoriasis and eczema treatments are focused on managing the condition and may need repeated use of medications to keep them at bay.
Conclusion
Skin covers our entire body and is integral to our overall body function. Without it, we would be dehydrated, fighting off infections constantly, and unable to maintain a stable body temperature.
Poor skin condition is often a warning sign that something else is wrong. It can be due to bad lifestyle habits, genetics, autoimmune diseases, hormonal changes, or environmental factors. Knowing the causes of skin conditions prepares us to take preventive steps to either avoid skin disorders or at least mitigate the effects.
Many skin conditions are chronic and may last a long time. Fortunately, there are a range of treatment methods which are readily available for patients. From pills taken orally to topical ointments and laser treatments for pigmentation, there are many different ways to cope with skin diseases of differing severities.
So if you develop a skin condition, do not despair. There are already numerous research studies on treatment methods and more findings are coming out everyday. To help with chronic or severe skin conditions, you should visit a dermatologist for a professional consultation. Qualified and trained in the field, they are the recommended people to talk to for advice and to receive treatment for skin disorders.
Thomson Specialist Skin Centre is a skin clinic in Singapore providing quality care for our patients. We provide a wide range of outpatient medical services. Our experienced skincare specialists are accredited with the Ministry of Health and are able to provide dermatological care with a patient-centric approach. Contact us today to find out more about our clinic and book an appointment with us online.

